Cell Culture Contamination Troubleshooting
Overview
Types of Contamination
Common Causes and Prevention of Contaminants
Microbial (bacteria, fungi, yeast)
Mycoplasma
Viral Contamination
Chemical Contamination
General Tips and Techniques
Working within the Biological Safety Cabinet
Pipetting and Prevention of Aerosols
Disinfection
How to Perform Routine Monitoring of Healthy Cells
Culture Contamination: An Overview
Although "cell culture contamination" typically conjures thoughts of bacteria among cells and cloudy media, unwanted invaders in the culture flask can take many forms. Viral and chemical contaminants can also have considerable consequences for culture health, and ensuring that cell lines are not cross-contaminated is critical to reproducibility of results.
How pervasive is cell contamination? Based on studies by the FDA, ATCC, and others, it is estimated that 5 – 30% of all cell cultures today are contaminated with mycoplasma species alone. Incidence of viral contamination of common cell lines exceeded 25% in one study5, and non-cytopathic viruses are even more likely than mycoplasma to escape detection, as culture health may not provide clues to their presence.
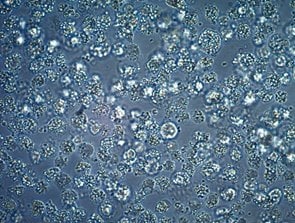
Figure 1.Cell Contamination
The key to controlling a specific contaminant is sometimes related to the ease with which it is detected. Bacterial, fungal, and yeast contaminants are often visible to the unaided eye, and may quickly kill the cells in culture, but subtle morphology may make significant microbial intruders like mycoplasma more difficult to identify. By comparison, viruses cannot be detected at all by conventional light microscopy, and their discovery is therefore often prompted by observations of unexplained detachment or other signs of poor cell health or even cell death.
One of the most significant concerns confronting the biology community in recent years is the contamination or even outright misidentification of research cell lines. For more on this important topic, click here to understand the causes and prevalence of cross-contaminated cell lines, and how to evaluate the integrity of cell line identity.
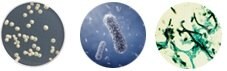
Bacterial, fungal (including molds), and yeast contamination are usually visible to the unaided eye as rapid-onset turbidity and color change of the culture medium (provided that the medium is supplemented with phenol red, the most common non-toxic pH indicator). Standard light microscopy will also reveal bacterial cells and fungal structures, so daily microscopic observation of cultures will ensure early detection of microbial contamination and enable appropriate action to be taken as soon as the first signs become apparent. In particular, prompt removal of contaminated cultures is needed to protect neighboring cultures, as well as the sterile tissue culture environment including culture incubators, baths, and the biosafety cabinet. Additionally, specific testing for bacteria and fungi should be used as part of a routine and regular quality control screening procedure.
Common Causes and Prevention of Microbial Contamination
Mycoplasma are a genus of bacteria that do not possess cell walls, and are therefore unaffected by antibiotics that limit bacterial growth by inhibiting cell wall formation. Their flexible morphology and cell size in the 0.15 to 0.3 µm range mean that they may escape standard cell culture filtration approaches that often use filters with 0.22 µm pores. Unlike most other bacterial contaminants, mycoplasma will not be apparent by casual inspection, and are difficult to detect by light microscopy due to their morphology and notably small size. Mycoplasma titer in culture can attain 108 organisms/mL without causing turbidity of the medium. They do not usually kill the mammalian cells they infect, but significantly impact cultures by altering cellular metabolism, causing chromosomal aberrations, slowing cell growth, and interfering with cell attachment. In short, they are likely to dramatically influence the results of most experiments performed using affected cell lines.
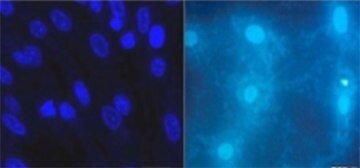
Figure 2.Common DNA detection agents such as DAPI or Hoechst reveal the presence of mycoplasma in contaminated cultures (right) using fluorescent microscopy.
The varied sources of mycoplasma contamination in the laboratory can present a challenge. As certain mycoplasma species are found on human skin, they can be introduced through poor aseptic technique, in addition to introduction via contaminated supplements such as fetal bovine serum. Mycoplasma are highly transmissible among neighboring contaminated cell cultures. Filtering media and buffers with membranes having pores 0.1 µm or less is necessary for mycoplasma treatment, as standard media filtration devices with pores of 0.22 or 0.45 µm will fail to exclude these small organisms.
Preventing, Detecting, and Eliminating Mycoplasma Contamination
Once mycoplasma contaminates a culture, it can quickly spread to other areas of the lab. Strict adherence to good laboratory practices is key, and routine testing for mycoplasma is highly recommended for successful control of mycoplasma contamination. The three most popular methods for detection include mycoplasma culture, DNA staining method and PCR based detection. We offer a variety of solutions for Mycoplasma Detection and Elimination. It is critical to establish a routine for mycoplasma screening of cultures even if you do not suspect the presence of this contaminant in the lab.
Preventing microbial contamination: are antibiotics the answer? One in tissue culture is the routine use of antibiotics, either alone or in cocktails with antifungals. Just as with therapeutic antibiotics prescribed by physicians, the continuous or inappropriate use of antibiotics can lead to the development of resistant strains that are difficult to eradicate and may require the use of later-generation antibiotics that may be toxic to the cell cultures. Recent studies have raised additional concerns about the potential for altered gene expression in cultured cells in the presence of antibiotics. |
Viral Contamination
Viruses are among the most difficult cell culture contaminants to detect in culture, requiring microscopy methods that would be impractical for most research laboratories. They can originate from the patient or host animal cell source, and several cell lines of biotechnological significance have been shown to contain endogenous retroviruses. More often, cells become infected by viruses present in animal-derived materials used to culture them. The small size of viruses makes them very difficult to remove from media, sera, and other solutions of biological origin. However, because most viruses are host- and even tissue-restricted, this may limit their capacity for cross-species or cross-tissue infection. Although viruses may be more common in cell cultures than many researchers realize, they may or may not present a significant confounder to cell culture if they do not induce cytopathic or other adverse effects on cells.
Beyond their potential to impact cultured cells, a major concern of using virally infected cell cultures is the potential health hazard they pose for laboratory personnel. Special safety precautions should always be used when working with tissues or cells from humans or other primates to avoid possible transmission of viral infection (HIV, hepatitis B, Epstein-Barr, simian herpes B virus, among others) from the cell cultures to laboratory personnel. Institutional environmental safety officers should be consulted regarding procedures for working with potentially hazardous tissues, cultures, or viruses. For more on risk assessment for laboratory personnel working with cell culture, click here
Best practices for reducing the incidence of viral contamination of cell cultures:
*Limit the number of biological sources (suppliers, animals) from which cells are extracted.
*Select animals/cells which are less virus-susceptible.
*Source cells from repositories that perform virus testing and provide certification of virus-free cell lines.
Chemical Contamination
Any nonliving contaminant of cell culture is often classified as a ‘chemical’ contaminant. These contaminants may originate from reagents or water used in media or buffers, or from equipment and supplies. Examples include free radicals, metal ions, disinfectant/detergent residues, or even endotoxins that persist after upstream bacterial contaminants are no longer present.
Tips for preventing chemical contamination:
*Always use laboratory-grade water for preparing buffers and solutions, and resuspending lyophilized reagents.
*Any reusable labware must be rinsed exhaustively and air-dried—autoclaving will have no effect on detergent residue.
*Obtain media, supplements, and serum (FBS, FCS) exclusively from suppliers that provide endotoxin testing certification.
General Tips and Techniques for Preventing and Eliminating Contamination
Working Within the Biological Safety Cabinet
When working within the biosafety cabinet, it’s helpful to remember that the air-flow is key to helping maintain a sterile environment. Both the rear and front vents should be kept clear at all times to achieve effective airflow. Before any practical procedure, the cabinet should be stocked with all required materials in order to minimize the potential for transfer of contaminants on the operator’s sleeves and hands.
At least twenty minutes should elapse after airflow is initiated before placing items to be used in the cabinet. All items that enter the cabinet must be sprayed first with 70% (v/v) sterile alcohol and wiped with lint-free wipes to prevent dust and particulates from entering the cabinet. Ensure airflow is well-established before any tops or containers are opened, to allow the airflow to purge the work area of particulates that may have been introduced.

Figure 3.Working in Safety Cabinet
Pipetting and Prevention of Aerosols
Disposable plastic pipettes—also called serological pipettes, available in capacities from 1-100 mL—are indispensable tools for cell culture. These must be individually-wrapped to ensure sterility. Adherence to the following guidance can minimize contamination and safety risks associated with pipetting.
- Use automatic pipette aids, with each pipette aid restricted for use in a single cabinet. To avoid contamination, disassemble and disinfect the pipette aid parts regularly. Ensure that pipette aid filters are kept well stocked and changed regularly.
- Use plugged pipettes (plugged at the top with cotton) whenever possible, especially when transferring medium. Avoid drawing liquid into the pipette plug. If plug is accidentally wetted, change pipette aid filter immediately.
- Avoid touching serological pipette altogether by unwrapping partially, fitting end to pipette aid, then removing paper sleeve.
- To avoid generating contaminating aerosols, do not create bubbles in the medium or pipette.
Disinfection
Methods designed for the disinfection/decontamination of culture waste, work surfaces and equipment must not only minimize contamination risk, but be safe for lab personnel. Always wear appropriate personal protective equipment (PPE) such as gloves and eye protection when using concentrated forms of disinfectants. Selected gloves should protect against the substance being handled. Manufacturers’ charts will help to identify the best gloves for a given task. Major disinfectants fall into groups, and their relative merits can be summarized as follows:
Sodium Hypochlorite or Bleach
- Good general purpose disinfectant
- Active against viruses
- Corrosive against metals—should not be used on metal surfaces such as centrifuges
- Readily inactivated by organic matter and should therefore be made fresh frequently
- Use commercial bleach to create a 10% (v/v) solution in waste liquid or for surface disinfection
Alcohol (e.g. Ethanol, Isopropanol)
- Effective concentrations: 70% for ethanol, 60-70% for isopropanol
- Effective against bacteria. Ethanol is effective against most viruses, but not non-enveloped viruses
- Isopropanol is not effective against viruses
- Aldehydes are irritants, and their use should be limited
Phenolic-based disinfectants should be avoided, as they are not supported as part of the EU Biocidal Products Directive review program.
How to Perform Routine Monitoring of Healthy Cells
Monitoring cell cultures is an important part of everyday cell culture. This tutorial will help explain the basics of monitoring your cells, including what a healthy culture looks like, cell confluency, and the different phases of cell culture growth. This video will also show common indicators of bacterial and mycoplasma contamination.
Related Products
References
To continue reading please sign in or create an account.
Don't Have An Account?